Publications
Have you ever been called a ‘CONSUMER EXPERT’? by Trish Lord
5 February 2019
Several of us (HCCA reps) played this role in mid-December, as part of the Chronic Disease Management Symposium in December 2018. This is an education and development opportunity for all Canberra Health Services staff.
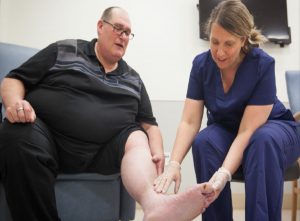 It’s an annual event run by the Chronic Disease Management Unit (CDMU). It was entitled “The Stigma of Obesity: Exploring the Barriers to Quality Health Care”. The morning sessions included various presentations:
It’s an annual event run by the Chronic Disease Management Unit (CDMU). It was entitled “The Stigma of Obesity: Exploring the Barriers to Quality Health Care”. The morning sessions included various presentations:
- Obesity Stigma and Bias: a consumer’s perspective
- Obesity: everybody’s problem, nobody’s responsibility
- What is Obesity and how can clinicians work effectively with patients?
Each small group comprised approximately 15 health care workers, including a facilitator and a scribe. We worked through three scenarios (2 negative and 1 positive), based on the actual experiences of obese consumers.
For each scenario, two members of the small groups volunteered to be the ‘clinician’ or the ‘patient’. They ‘played their role’ according to background information, which I also had. The consumer expert’s role was to share their ideas on what health care providers can do to reduce the barriers and weight-related stigma for patients with obesity accessing health care. I found it most interesting to see how the actors carried out their roles, and to hear the feedback from the actors and observers after each scenario.
During the two negative scenarios, it was obvious to the group how poorly the ‘health professional’ was interacting with the patient. The ‘clinicians’ admitted how badly they felt behaving this way. And the ‘patients’ expressed their overwhelming disappointment and frustration, verging on rejection, through the way they were treated.
Barriers and stigmas discussed included:
- judgemental questions and statements,
- impersonal interactions with health care workers,
- lack of response to big hints from consumer,
- dismissive, bossy or disinterested behaviour,
- a lack of extra information,
- distracted body language,
- lack of eye contact, and
- comparisons with other people.
The positive scenario was relief to all. The ‘patient’ felt safe with the ‘clinician’ who accepted their status and maintained eye contact. It also helped when the ‘clinician’ provided feedback through supportive questions and information, active listening, and opportunities for follow-up.
In particular, I mentioned ‘reflective listening’ that can be so empowering in counselling. Through practice, it can become a natural behaviour in the way we all communicate with each other.
By the end, I am sure we all had a better understanding of the challenges, and of practical steps that could reduce barriers and stigmas in our practices and life skills.
by Trish Lord
HCCA Member

